Three months ago, Mark, a dedicated architect, decided it was time to gradually taper off Effexor after years of managing his anxiety. He'd done his homework, discussed it with his doctor, and felt prepared for some discomfort. Yet, the initial days of reducing his dose were a blur of unexpected sensations - the sudden surges of anxiety he hadn't felt in years, the dizzy spells that made walking a straight line a challenge, and the peculiar 'brain zaps' that startled him awake. He quickly realized that coming off medication isn't just about reducing a pill count; it's a profound journey of recalibrating the brain. Understanding what to expect from Effexor withdrawal became his anchor in a sea of uncertainty.
Effexor withdrawal, clinically known as venlafaxine discontinuation syndrome, typically presents with a range of physical and psychological symptoms that can emerge within 24-48 hours of stopping or significantly reducing the medication. These can include dizziness, nausea, headaches, mood swings, and those peculiar 'brain zaps.' While symptoms usually improve within three weeks, they can sometimes linger longer. Getting informed is the first, crucial step.
The Reality of Effexor Withdrawal
When you reduce or stop taking Effexor (venlafaxine), your brain undergoes a significant neurochemical adjustment. This happens because Effexor, a serotonin-norepinephrine reuptake inhibitor (SNRI), affects the balance of neurotransmitters like serotonin and norepinephrine. When this balance shifts too quickly, your brain needs time to adapt, leading to a cascade of withdrawal symptoms. This isn't a sign of addiction in the traditional sense, but rather a physiological response to the change in medication levels (Gabriel & Sharma, 2017).
Healthcare providers often recommend a gradual tapering schedule to minimize these effects, yet even with careful planning, some symptoms may still surface. It's a testament to the powerful connection between our mental health and our brain's intricate chemistry. And it's why knowing what to expect from this process is so vital for anyone considering a change.
Unraveling the Withdrawal Timeline
So, what to expect from Effexor withdrawal as it unfolds? Everyone's experience is unique, influenced by factors like the dosage you were on and how long you've been taking the medication. But there's a general pattern most people follow:
- Early Symptoms (24 to 48 hours): The first signs often emerge quickly. Think flu-like symptoms, a creeping anxiety, or a feeling of agitation that wasn't there before. For someone like Sarah, who missed a dose while traveling, this might manifest as sudden irritability during a layover, making an already stressful situation worse.
- Peak Symptoms (Days 3 to 7): This is often when symptoms are most pronounced. Dizziness, persistent nausea, and a general sense of unease can be particularly challenging. Imagine trying to focus on work when every head movement brings a wave of vertigo.
- Improvement Phase (Week 2): Thankfully, for many, the intensity begins to lessen during the second week. Physical symptoms often start to recede, though some psychological discomfort might still linger. You might feel a glimmer of your old self returning.
- Recovery Period (Week 3 and Beyond): By the third week, most physical symptoms tend to resolve. However, emotional fluctuations, such as mood swings or heightened irritability, can sometimes persist for a longer duration. It's a reminder that healing isn't always linear.
It's worth noting that not everyone experiences withdrawal. Research suggests that around 33% to 56% of people taking antidepressants may experience discontinuation symptoms when they stop their medication (Henssler et al., 2024).
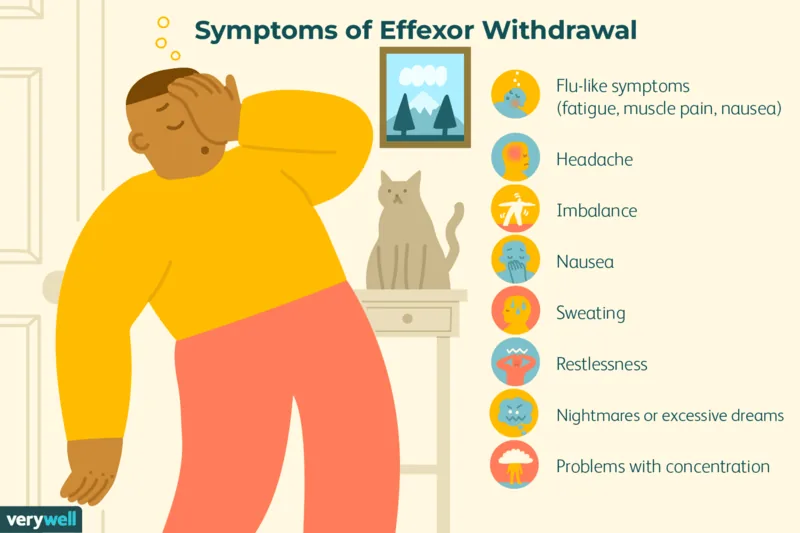
The Symptoms: What It Feels Like
It's natural to wonder, beyond the clinical definitions, what to expect from the actual *feeling* of withdrawal. As your brain readjusts to the absence of the medication, a range of sensations can arise:
- Agitation or irritability
- Anxiety
- Changes in appetite (either increased or decreased)
- Confusion or difficulty concentrating
- Dizziness or lightheadedness
- Headaches, sometimes intense
- Mood changes, including sudden shifts or emotional sensitivity
- Nausea or vomiting
- Nightmares, vivid dreams, or other sleep disturbances
- Paresthesias (a prickling, tingling, or 'pins and needles' sensation)
- Sweating, often in sudden bursts
'Brain Zaps': A Peculiar Sensation
One of the most distinctive and often alarming symptoms people report are 'brain zaps,' sometimes called 'brain shivers.' These are typically described as very brief, repetitive, electric shock-like feelings confined to the head or brain (Papp & Onton, 2018). For example, Liam recalled feeling a distinct 'zap' whenever he turned his head quickly, accompanied by a fleeting sense of disorientation, almost like a brief circuit overload.
These sensations can spread to other parts of the body and are often accompanied by tinnitus (ringing in the ears) or vertigo. While unsettling and disruptive to daily life, current evidence suggests brain zaps themselves are not dangerous. Understanding what to expect from these sensations can help mitigate alarm.
Navigating the Journey: Coping Strategies
Effexor withdrawal symptoms can develop quickly, so if you miss a dose, it's generally best to take it as soon as you remember. If it's very close to your next scheduled dose, skip the missed one and stick to your regular schedule. The goal is to get back on track as soon as possible to stabilize your system. If you are intentionally discontinuing Effexor, there are several ways to make the withdrawal period more tolerable:
- Team Up with Your Healthcare Provider: Your doctor is your most vital ally. Discuss the benefits and risks of stopping, and work together to create a slow, gradual tapering plan. They can adjust the schedule based on your unique response.
- Ask About OTC Medications: Your doctor might suggest over-the-counter remedies to ease specific symptoms, such as anti-nausea medication, sleep aids, or pain relievers for headaches.
- Consider Psychotherapy: Engaging in therapy during discontinuation can significantly decrease your risk of a depression relapse (Harvard Health Publishing). A therapist can help you process emotions and develop coping mechanisms for any returning symptoms.
- Seek Support: Let a trusted friend or family member know what you're going through. Having someone understand and offer practical help - like reminding you about a dose or simply listening - can make a huge difference. For instance, Mark found immense comfort in his partner's patience and understanding during his mood swings.
- Keep Up with Follow-Ups: Regular check-ins with your healthcare provider are crucial, both during the taper and after you've stopped. This ensures any concerns are addressed promptly and adjustments can be made.
- Practice Self-Care: During withdrawal, prioritizing self-care is more important than ever. Gentle exercise, nutritious meals, consistent sleep, and stress management techniques like meditation or deep breathing can help stabilize your mood. Emily, for example, found her daily morning yoga and journaling routine to be an invaluable anchor, helping her ground herself amidst the internal shifts.
When to Seek Help: Important Warnings
While most withdrawal symptoms are manageable, some can be severe and require immediate medical attention. The disorientation that can accompany withdrawal, for instance, can be dangerous if you're driving or operating machinery.
In rare cases, stopping Effexor abruptly can lead to severe and frightening reactions. If you or someone you love experiences any of the following, call 911 or seek emergency medical help right away:
- Delirium (severe confusion and disorientation)
- Suicidal feelings or thoughts
- Psychosis (loss of contact with reality, hallucinations, delusions)
If you are experiencing suicidal thoughts, please reach out for support. Many resources are available to help. If you experience worsening anxiety or depression during withdrawal, and these symptoms last more than a month, it may indicate a relapse, suggesting a need for ongoing mental health treatment. Always talk to your care provider if you have any concerns.
Beyond Withdrawal: Long-Term Management
Once you've made the decision to stop your antidepressant, the temptation might be to just toss out the remaining pills. Instead, commit to a slow, deliberate process with your physician. How you'll taper will depend on several factors, including how long you've been on the drug, your current dose, any past experiences with withdrawal, and your overall health.
Sometimes, even with the most careful and gradual tapering, withdrawal symptoms can still emerge. In these instances, your physician might suggest a temporary switch to another antidepressant, like Prozac (fluoxetine), to help ease the transition (Shapiro & Cohrs, 2025). Prozac has a longer half-life, meaning its concentration in the body decreases more slowly, which can help smooth out the discontinuation process and reduce bothersome withdrawal effects.
And knowing what to expect from these potential long-term scenarios allows for proactive planning. Remember, you're not alone. Many individuals find comfort and practical advice by connecting with others who have navigated similar experiences. Organizations like the National Association for Mental Illness (NAMI) or the Anxiety and Depression Association of America (ADAA) often host online discussion groups where you can share stories and find mutual support.