The constant urge to sanitize your hands until they're raw, the nagging feeling that every surface is a breeding ground for illness, the avoidance of social gatherings for fear of unseen threats - these aren't just quirks; they can be hallmarks of mysophobia, an intense and often debilitating fear of germs and contamination. This pervasive anxiety can shrink your world, making everyday activities feel like perilous expeditions. But what if you could navigate your day with less fear and more freedom? Understanding the roots of mysophobia and implementing practical coping strategies can pave the way for a more balanced and fulfilling life, allowing you to manage your fear of germs effectively.
Understanding Mysophobia (Germophobia)
Mysophobia, commonly known as germophobia, is more than just a preference for cleanliness; it's an overwhelming and irrational fear of germs and contamination. While a normal concern for hygiene is healthy, mysophobia escalates these worries to a level that significantly disrupts daily life. This phobia can manifest as extreme avoidance behaviors, obsessive cleaning rituals, and a pervasive sense of dread associated with dirt or potential exposure to pathogens.
This condition is also referred to by other names, such as bacillophobia or bacteriophobia, all pointing to the core fear of microscopic organisms. It's often associated with obsessive-compulsive disorder (OCD) due to overlapping symptoms like compulsive cleaning, but it can exist independently. The fear of germs can affect anyone, regardless of background, and its impact can be profound.
Recognizing the Signs and Symptoms
The most evident signs of mysophobia revolve around behaviors designed to prevent germ exposure. These often include:
- Avoiding places perceived as germ-ridden, such as public restrooms, subways, or crowded spaces.
- An intense, persistent fear of becoming contaminated by germs, dirt, or bodily fluids.
- Excessive hand washing, scrubbing, or using hand sanitizer to the point of skin damage.
- Obsessive thoughts about cleanliness, contamination, and the potential for illness.
- Overuse of cleaning products, disinfecting surfaces repeatedly.
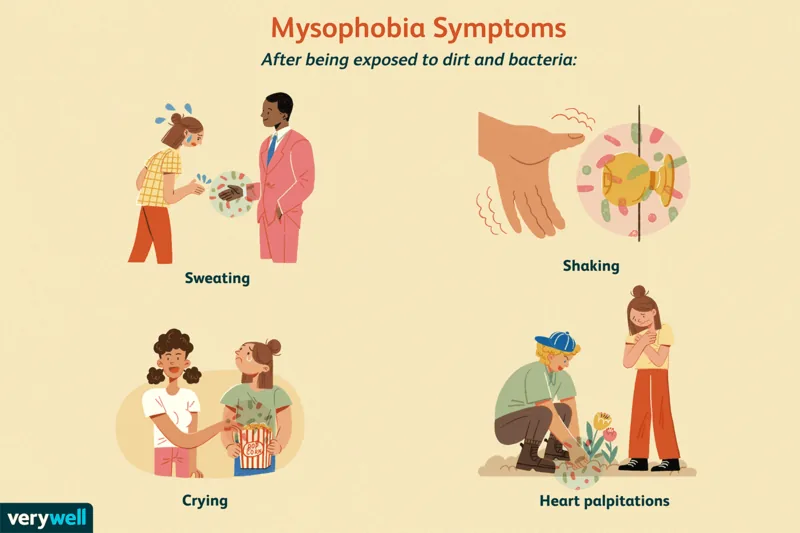
When confronted with perceived contamination, individuals might experience acute anxiety. These reactions can include physical symptoms like shaking, sweating, rapid heart palpitations, and even crying. The trigger might be direct contact, like shaking hands, or even the mere thought of potential exposure, such as touching a public doorknob.
Daily life can become a minefield. You might find yourself showering multiple times a day, refusing to share food or utensils, or avoiding public transportation altogether. This constant vigilance takes an immense toll, both mentally and physically.
Diagnosing Mysophobia
Distinguishing mysophobia from a general dislike of dirt is crucial. It's characterized by an intense, excessive fear that drives significant avoidance of people, objects, or situations that could lead to contamination. While mysophobia isn't listed as a standalone diagnosis in the DSM-5-TR, it's typically classified as a specific phobia if it meets certain criteria (American Psychiatric Association, 2013).
For a diagnosis of specific phobia, the symptoms must:
- Cause significant distress or avoidance.
- Trigger an immediate anxiety response upon exposure to the feared stimulus.
- Involve a fear that is unreasonable or excessive in proportion to the actual danger.
Crucially, these symptoms must impair a person's ability to function normally in various aspects of their life, such as work, social relationships, or self-care. The phobia must also persist for at least six months and not be better explained by another mental disorder (National Institute of Mental Health).
Unpacking the Causes and Risk Factors
The precise origins of mysophobia aren't fully understood, but a combination of factors likely contributes to its development. These can include:
- Genetics: A family history of anxiety disorders or phobias may increase susceptibility (Meier & Deckert, 2019).
- Brain Structure and Function: Certain neurological differences might play a role in anxiety development.
- Traumatic Experiences: A past event involving illness, contamination, or a perceived threat of germs can trigger or exacerbate the phobia. For example, a severe childhood illness requiring extensive medical procedures could lead to a lifelong fear of germs.
- Learned Behaviors: Witnessing germ-averse behaviors in family members or being exposed to cultural narratives emphasizing extreme cleanliness can influence the development of the phobia.
- Co-occurring Mental Health Conditions: Mysophobia often exists alongside other conditions like OCD, anxiety disorders, or depression, with studies showing a significant overlap (Eaton et al., 2018).
The fear of germs can be particularly intertwined with OCD. While both may involve compulsive handwashing, the motivation differs. In OCD, it might be to alleviate obsessive thoughts, whereas in mysophobia, it's a direct response to the perceived need to eliminate germs. This subtle distinction underscores the importance of professional assessment.
Effective Treatments for Coping Fear of Germs
Fortunately, mysophobia is a treatable condition. Seeking professional help is the most effective first step, as the phobia can intensify over time. The primary treatment approaches include psychotherapy and, sometimes, medication.
Psychotherapy is the cornerstone of treatment. Two highly effective methods are:
- Cognitive Behavioral Therapy (CBT): This therapy helps individuals identify and challenge the negative thought patterns and beliefs that fuel their fear. By restructuring these thoughts, people can develop more balanced perspectives on contamination and risk.
- Exposure Therapy: This gradual process involves controlled and safe exposure to feared situations or objects. Starting with minimal exposure and progressively increasing it, individuals learn to manage their anxiety response, demonstrating that their feared outcomes don't occur or are manageable. This is a key strategy for coping with fear of germs.
Virtual reality (VR) exposure therapy has also shown promising results, offering a controlled environment for exposure that can be as effective as real-world scenarios (Wechsler et al., 2019). Online therapy platforms can also provide accessible support and CBT-based interventions.
Medication is typically not the primary treatment for specific phobias like mysophobia. However, it may be prescribed to manage severe anxiety symptoms or treat co-occurring conditions such as depression or generalized anxiety disorder. Medications like D-cycloserine have been explored to enhance the effectiveness of exposure therapy, but they are usually used in conjunction with psychotherapy (Thng et al., 2020).
Practical Strategies for Managing Mysophobia
Beyond professional treatment, several self-help strategies can significantly aid in coping with the fear of germs:
- Mindfulness and Meditation: Practicing mindfulness helps you stay present and observe your anxious thoughts without judgment, reducing their power.
- Deep Breathing Exercises: Simple techniques like diaphragmatic breathing can calm the nervous system during moments of anxiety (Zaccaro et al., 2018).
- Regular Exercise: Physical activity is a proven stress reliever and mood booster.
- Adequate Sleep: Prioritizing sleep is crucial for emotional regulation and resilience (Davidson & Pace-Schott, 2020).
- Gradual Self-Exposure: Gently challenge your avoidance behaviors in small, manageable steps. For instance, if you avoid public transport, start by sitting on a stationary bus for a few minutes.
- Support Groups: Connecting with others who understand your struggles can provide invaluable emotional support and practical advice.
Remember, the goal isn't to eliminate all concern about hygiene but to reduce the fear to a manageable level, allowing you to live a fuller life. Effective coping with fear of germs involves a multi-faceted approach combining professional guidance with personal commitment to these strategies.
Sources: American Psychiatric Association, 2013; Davidson & Pace-Schott, 2020; Eaton et al., 2018; Meier & Deckert, 2019; National Institute of Mental Health; Thng et al., 2020; Wechsler et al., 2019; Zaccaro et al., 2018.